Prior to 2021, Japanese encephalitis virus (JEV), which causes inflammation of the brain, had only ever affected five people in Australia (McGuinness et al. 2023).
All of these cases were locally acquired in far-north Queensland in 1995 and 1998 (McGuinness et al. 2023).
In 2021, a sentinel case of JEV led to an unprecedented outbreak of the virus in 2022, with infections being acquired as far south as New South Wales, South Australia and Victoria - where it had never before been detected (McGuinness et al. 2023; Pendrey & Martin 2023).
This outbreak resulted in 45 infections and 7 deaths between January 2021 and December 2022 (DoHaAC 2023a).
The surge in cases was believed to be associated with climate change and flooding, which encouraged waterbirds to migrate to newly formed inland waterways. The warm, wet conditions also facilitated an increase in the mosquito population (Lanese 2022).
Most recently, six JEV cases have been notified in Australia since December 2024. These are the first new human infections since the 2021-2022 outbreak (CDC 2025).
While JEV is no longer considered a Communicable Disease Incident of National Significance in Australia (DoHaAC 2023a), it’s crucial for healthcare professionals to remain up-to-date with the latest information on this virus.
So, what exactly is Japanese encephalitis, and should there be cause for concern in the community?
What is Japanese Encephalitis?
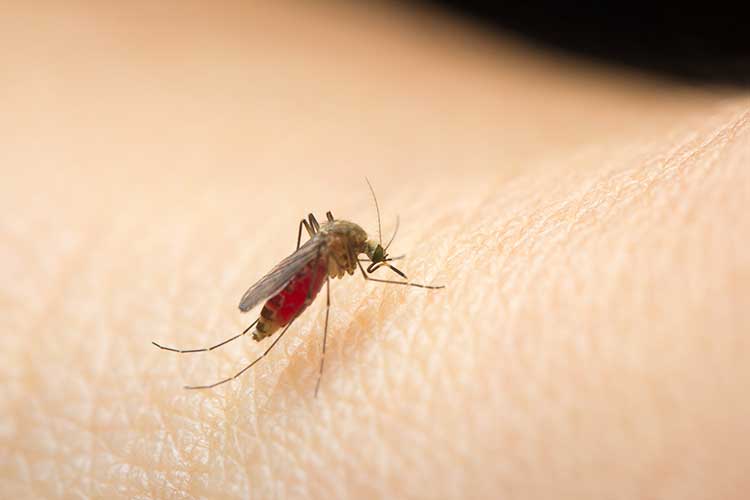
Japanese encephalitis is a mosquito-borne illness caused by the Japanese encephalitis virus (JEV) (NSW Health 2024).
Like other types of encephalitis such as Murray Valley encephalitis, Japanese encephalitis is an inflammation of the brain. While 99% of cases are asymptomatic, severe cases can lead to lifelong disability or even death (Healthdirect 2024; Queensland Government 2025).
What Causes Japanese Encephalitis?
JEV is a zoonotic virus, meaning it’s spread from animals to people. However, animals can’t spread the virus to humans directly, nor can humans spread the virus to other humans. Instead, mosquitoes that feed on infected animals acquire the virus themselves and become vectors (i.e. living organisms that transmit pathogens from infected animals to other animals, or humans). If an infected mosquito feeds on a human, the virus will be transmitted to that individual (Davey 2022; Australia Wide First Aid 2022; EFSA 2023).
Only Culex genus mosquitoes, predominantly the Culex annulirostris species, can transmit the illness (Lanese 2022; Business Queensland 2025).
The JEV virus is predominantly found in pigs and waterbirds (particularly herons and egrets), which are amplifying hosts. This means they facilitate the rapid multiplication of infectious agents and can reinfect new mosquitoes. Therefore, the virus is maintained in nature through mosquito-waterbird or mosquito-waterbird-pig transmission cycles (Business Queensland 2025; Biology Online 2021).
Humans and other animals, on the other hand, are ‘dead-end’ hosts that once infected do not play any further role in transmission (VIC DoH 2025).
Other animals that can be infected with JEV include:
- Horses
- Cattle
- Sheep
- Dogs
- Cats
- Bats
- Rodents
- Reptiles
- Amphibians
- Birds.
(Business Queensland 2025)
Excluding pigs and horses, animals infected with JEV are usually asymptomatic. Signs of JEV in pigs typically include mummified, stillborn or weak piglets, possibly with neurological issues, and in horses, fever, jaundice, lethargy, anorexia and neurological issues (Department of Agriculture, Fisheries and Forestry 2025).
It’s not possible for humans to contract JEV by touching infected animals or eating animal products such as pork (NSW Health 2024).
Risk Factors for Japanese Encephalitis
Those at most risk of locally-acquired infection in Australia are people in close proximity to infected animals and mosquitoes. These include:
- Those who work at, visit or live close to piggeries or abattoirs
- Those participating in outdoor activities like camping, fishing or hiking in high-risk areas
- Those who work directly with mosquitoes (e.g. environmental health officers and entomologists)
- Diagnostic and research laboratory personnel working with mosquitoes or JEV cultures.
(NSW Health 2024; Queensland Government 2025)

Symptoms of Japanese Encephalitis
Only around 1% of JEV infections in humans are symptomatic (Queensland Government 2025). If symptoms do occur, they typically develop 5 to 15 days after being bitten by an infected mosquito. The individual might experience:
- Fever
- Headache
- Abdominal pain and vomiting.
(NSW Health 2024; Queensland Government 2025)
In severe cases, symptoms may include:
- High fever
- Chills
- Severe headache
- Stiff neck
- Disorientation
- Paralysis
- Tremors
- Coma
- Seizures.
(NSW Health 2024; Queensland Government 2025)
One-third of severe cases will result in death, and another third will result in permanent disability (Queensland Government 2025).
Diagnosis is typically made via a blood test or spinal fluid sample (SA Health 2024).
There is no specific treatment for Japanese encephalitis. Mild symptoms can be managed by resting, ensuring adequate fluid intake and taking paracetamol, while more severe cases may require admission to hospital for observation and supportive care (DoHaAC 2023b).
Preventing Japanese Encephalitis

A vaccine to protect against JEV is available and is offered for free to certain priority groups in Australia. For further information on who is eligible for free vaccination, refer to each state and territory’s Department of Health.
See the Australian Immunisation Handbook for more information on the JEV vaccine.
JEV can also be prevented by avoiding mosquito bites through strategies such as:
- Being careful outdoors during dawn, dusk and the evening, when Culex mosquitoes are most active
- Wearing light-coloured, loose-fitting, long-sleeved clothing, as well as covered shoes and socks, when outdoors
- Applying mosquito repellent that contains diethyltoluamide (DEET), picaridin or oil of lemon eucalyptus to all exposed skin (after sunscreen)
- Reapplying repellant after swimming
- Using flyscreens in the home
- Using flyscreens or mosquito nets when camping
- Using insecticide sprays, vapour dispensing units and mosquito coils to remove mosquitoes
- Removing water-holding containers around the home, as these are breeding grounds for mosquitoes.
(NSW Health 2024; DoH 2023b)
Test Your Knowledge
Question 1 of 3
Which one of the following best describes how Japanese encephalitis virus is transmitted to humans?
Topics
Further your knowledge
 Free
Free Free
Free Free
Free Free
Free Free
FreeReferences
- Australian Centre for Disease Control 2025, ‘Protect Yourself From Japanese Encephalitis Virus’, Australian Centre for Disease Control News, 28 February, viewed 25 March 2025, https://www.cdc.gov.au/newsroom/news-and-articles/protect-yourself-japanese-encephalitis-virus
- Australia Wide First Aid 2022, Japanese Encephalitis Virus Threat, Australia Wide First Aid, viewed 25 March 2025, https://www.australiawidefirstaid.com.au/resources/japanese-encephalitis
- Biology Online 2021, Amplifier Host, Biology Online, viewed 25 March 2025, https://www.biologyonline.com/dictionary/amplifier-host
- Business Queensland 2025, Japanese Encephalitis, Queensland Government, viewed 25 March 2025, https://www.business.qld.gov.au/industries/farms-fishing-forestry/agriculture/livestock/animal-welfare/pests-diseases-disorders/japanese-encephalitis
- Davey, M 2022, ‘What is Japanese Encephalitis and Why is it Spreading in Australia?', The Guardian, 8 March, viewed 25 March 2025, https://www.theguardian.com/australia-news/2022/mar/08/what-is-japanese-encephalitis-and-why-is-it-spreading-in-australia
- Department of Agriculture, Fisheries and Forestry 2025, Japanese Encephalitis, Australian Government, viewed 25 March 2025, https://www.agriculture.gov.au/biosecurity-trade/pests-diseases-weeds/animal/japanese-encephalitis
- Department of Health and Aged Care 2023a, Statement on the End of Japanese Encephalitis Virus Emergency Response, Australian Government, viewed 25 March 2025, https://www.health.gov.au/news/statement-on-the-end-of-japanese-encephalitis-virus-emergency-response
- Department of Health and Aged Care 2023b, Japanese Encephalitis, Australian Government, viewed 25 March 2025, https://www.health.gov.au/diseases/japanese-encephalitis
- European Food Safety Authority 2023, Vector-Borne Diseases, European Union, viewed 25 March 2025, https://www.efsa.europa.eu/en/topics/topic/vector-borne-diseases
- Healthdirect 2024, Encephalitis, Australian Government, viewed 25 March 2025, https://www.healthdirect.gov.au/encephalitis
- Lanese, N 2022, ‘1st Major Outbreak of Japanese Encephalitis Hits Australia’, Live Science, 18 March, viewed 25 March 2025, https://www.livescience.com/australia-encephalitis-outbreak-climate-change
- McGuinness, SL, Lau, CL & Leder, K 2023, ‘The Evolving Japanese Encephalitis Situation in Australia and Implications for Travel Medicine’, J Travel Med., vol. 30, no. 2, viewed 25 March 2025, https://pmc.ncbi.nlm.nih.gov/articles/PMC10075061/
- NSW Health 2024, Japanese Encephalitis Fact Sheet, New South Wales Government, viewed 25 March 2025, https://www.health.nsw.gov.au/Infectious/factsheets/Pages/japanese_encephalitis.aspx
- Pendrey, C & Martin, GV 2023, ‘Japanese Encephalitis Clinical Update: Changing Diseases Under a Changing Climate’, Australian Journal of General Practice, vol. 52, no. 5, viewed 25 March 2025, https://www1.racgp.org.au/ajgp/2023/may/japanese-encephalitis-clinical-update
- Queensland Government 2025, Japanese Encephalitis, Queensland Government, viewed 25 March 2025, https://www.qld.gov.au/health/condition/infections-and-parasites/viral-infections/japanese-encephalitis
- SA Health 2024, Japanese Encephalitis - Including Symptoms, Treatment and Prevention, Government of South Australia, viewed 25 March 2025, https://www.sahealth.sa.gov.au/wps/wcm/connect/public+content/sa+health+internet/conditions/infectious+diseases/japanese+encephalitis/japanese+encephalitis+-+including+symptoms%2C+treatment%2C+and+prevention
- Victoria Department of Health 2025, Japanese Encephalitis, Victoria State Government, viewed 25 March 2025, https://www.health.vic.gov.au/infectious-diseases/japanese-encephalitis
 New
New 
