Rashes are an extremely common medical presentation, particularly in children (RCHM 2018).
In fact, skin conditions, including rashes, are one of the most common presentations in general practice, accounting for 17% of issues encountered (RACGP 2022).
Most rashes are temporary and not a cause for concern (HealthEngine 2017). Due to how common they are, they may simply be brushed off as ‘nothing serious’.
However, rashes have a diverse range of potential causes and presentations, and in some cases require immediate medical attention (RCHM 2018).
Rashes can be difficult to identify, and as a healthcare professional, being able to recognise potentially dangerous rashes is critical.
So, how can common rashes be differentiated, and when is there a cause for serious concern?
This Article will provide an overview of some common rashes, along with related Ausmed resources. Please note that this is not an exhaustive list.
What is a Rash?
A rash is an area of skin that has undergone a change in texture or colour and may appear irritated or inflamed. It may be localised, or affect the whole body (NCI 2020).
Rashes can present in a variety of ways. The affected area skin might appear:
- Discoloured (red, pink or purple)
- Warm
- Scaly
- Flat
- Bumpy
- Dry
- Itchy
- Swollen
- Painful
- Cracked
- Blistered
- Pus-filled.
(NCI 2020; Soyer & Lee 2018)
Common Rashes
Anaphylaxis
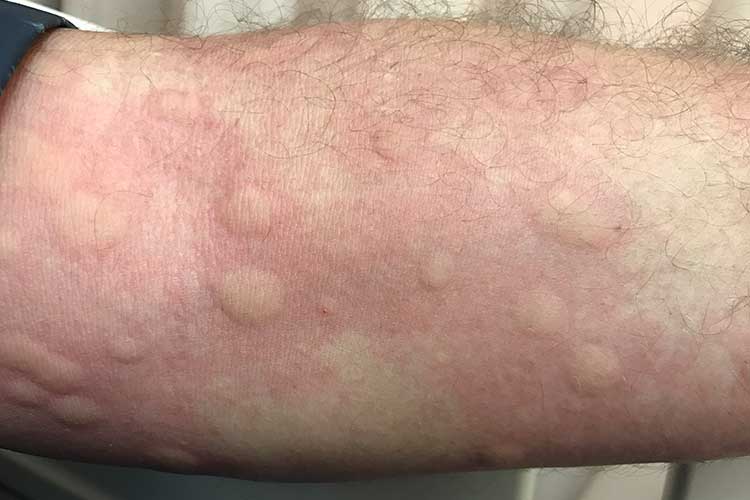
Type: Acute, potentially life-threatening reaction.
Cause: Exposure to an allergen, typically a food, medicine or insect.
Rash appearance: Hives or welts - raised, bumpy, itchy rash that may be red or closer to the person’s normal skin colour. Swelling may be present, and the skin can feel hot or flushed.
Symptoms:
Other signs of anaphylaxis include:
- Difficult or noisy breathing
- Swollen tongue
- Swollen or tight throat
- Swollen face, lips and/or eyes
- Difficulty talking or hoarse voice
- Wheezing or persistently coughing
- Persistent dizziness
- Collapse
- Abdominal pain and vomiting
- Pale appearance and floppiness (in children).
Treatment: Immediate intramuscular adrenaline is required if the patient is experiencing shock, airway swelling or breathing difficulties. This should be followed by transportation to acute care where fluid and oxygen may be administered if required.
Further information: Recognising and Treating Acute Anaphylaxis
(ASCIA 2024a; Gartside 2024; Queensland Government 2019)
Bites and Stings
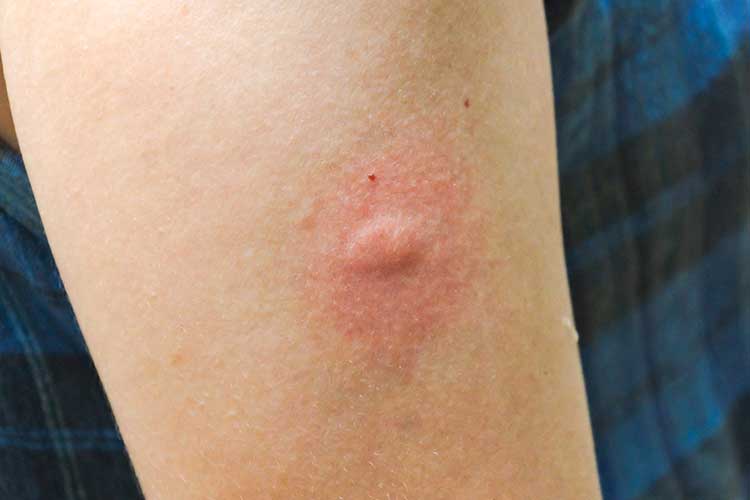
Note: Specific management of bites and stings will depend on the causative insect.
Type: Acute reaction.
Cause: An insect penetrating the skin and potentially leaving its saliva, faeces or venom in the body.
Rash appearance: Often, a bite or sting will cause localised redness, with a bump or blister surrounding the puncture site. If the person experiences an allergic reaction to the bite/sting, there may be localised swelling, or in the case of a more generalised reaction, redness, swelling or hives in other areas of the body. In the case of an anaphylactic reaction, they may present with hives or welts.
Symptoms:
- Irritation
- Itching
- Pain or a burning sensation
- Symptoms of an anaphylactic reaction (in severe cases).
Treatment: Mild bites and stings will generally heal on their own within 48 hours. Techniques such as taking cool baths and showers, wearing loose clothing and applying topical lotions or creams may help to relieve itching.
Further information: Basic First-Aid for the Envenomated Person (Snakes, Spiders and Insects)
(Healthdirect 2024a; Better Health Channel 2022)
Contact Dermatitis
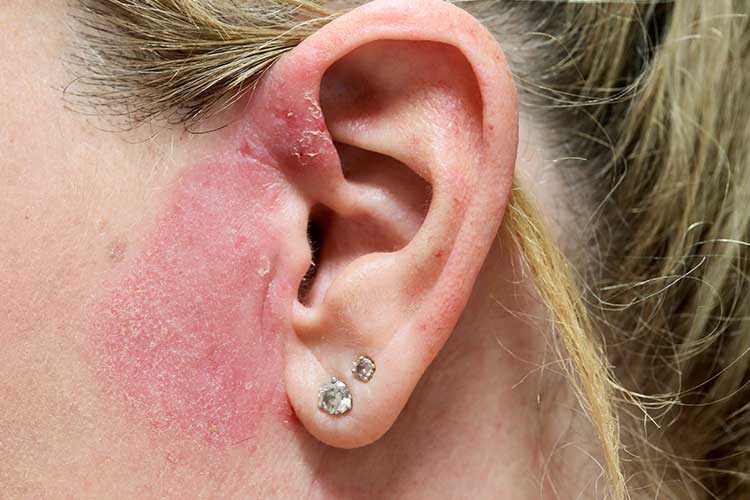
Type: Acute reaction.
Cause: Direct contact between the skin and an inflammation-causing stimulus. Common examples include nickel, chemicals, plants, cosmetics, perfumes and ointments. The rash generally occurs one to two days after the initial contact with the trigger.
Rash appearance: Cracked, red, blistered, thickened and dry skin, possibly with weeping.
Symptoms: Itching.
Treatment: The rash will gradually heal after the irritant is removed, within one to two weeks post-exposure. Symptoms may be treated with topical emollient moisturisers and steroid creams, or in the case of severe immune response, with oral medicines.
(ASCIA 2024b; Soyer & Lee 2018; Tate 2019)
Note: Healthcare workers are particularly susceptible to occupational contact dermatitis due to irritation from constant handwashing and the frequent use of gloves (Skin Health Institute 2023).
Eczema (Atopic Dermatitis)
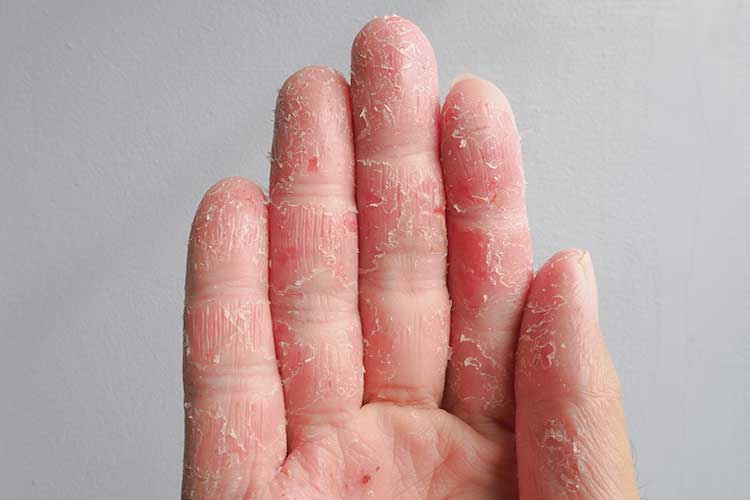
Type: Chronic condition.
Cause: The exact cause of eczema is not known, but it’s thought to be a combination of environmental triggers and genetic factors. People who have eczema have an overactive immune system that produces inflammation when triggered by a substance inside or outside of the body. Factors that may contribute to symptom flare-ups include:
- Allergens
- Stress
- Heat
- Certain materials and substances
- Animals or dust mites
- Infections
- Scratching
- Dry skin.
Rash appearance: Scaly, dry, red patches of skin. The affected area may form tiny blisters filled with clear fluid and weep. Commonly affected areas of the body include the cheeks, elbow creases and backs of the knees.
Symptoms: Severe itching during flare-ups, with the affected areas potentially becoming infected.
Treatment: The condition can be managed by keeping the skin moisturised and protected, avoiding known irritants, and avoiding scratching. Flare-ups are generally treated using topical corticosteroids or calcineurin inhibitors.
Further information: Eczema Symptoms and Management
(NEA 2025; ASCIA 2024c; Better Health Channel 2023a)
Herpes Zoster (Shingles)
Type: Acute viral infection, however, about 10% of people will experience chronic pain and tingling (post-herpetic neuralgia) for months or years after the infection.
Cause: Reactivation of the dormant varicella-zoster virus in people who have previously had chickenpox.
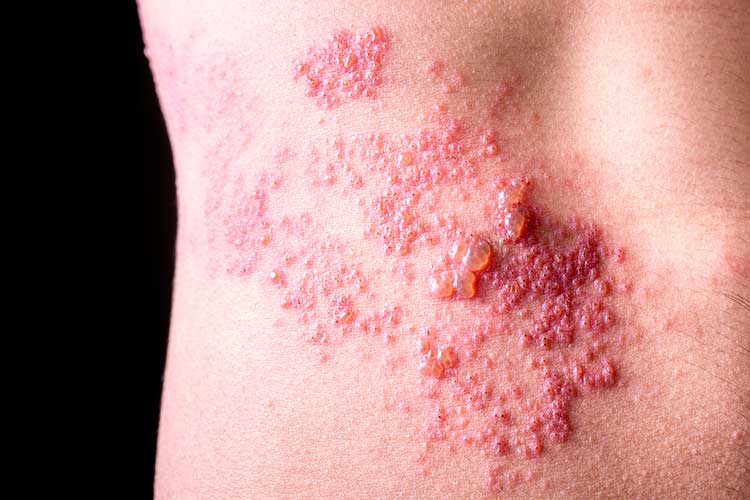
Rash appearance: Red rash with fluid-filled blisters that break open and crust over. The rash is typically only on one side of the body, on the face, chest, back, abdomen or pelvis.
Symptoms: On the affected area of the body, the person will initially experience pain, a burning, tingling, itching or stabbing sensation, sensitivity to touch, and numbness, as well as other symptoms like sensitivity to light, fatigue, fever and/or headaches. Two to three days after the onset of these symptoms, a rash will appear in the affected area.
Treatment: Shingles resolves on its own within two to six weeks. However, prescription antiviral medicines can be used to reduce the severity of symptoms and the risk of complications. Taking over-the-counter analgesics, keeping the rash dry and clean, avoiding scratching and wearing loose clothing may also assist in symptom management.
Further information: What Causes Shingles (Herpes Zoster)?
(Mayo Clinic 2022; Healthdirect 2023a)
Psoriasis
Type: Chronic inflammatory condition.
Cause: Skin cells growing too quickly. The exact cause of the condition is unknown, but it may have a genetic component. Factors such as smoking, excessive alcohol consumption, certain medicines, sun exposure, injury and certain infections (e.g. streptococcal tonsillitis) can exacerbate symptoms.
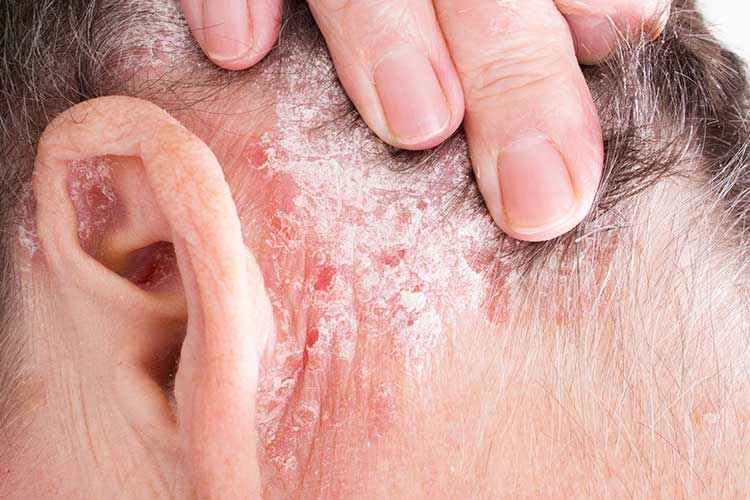
Rash appearance: Red, dry, plaques covered with silvery scales. The plaques have clearly defined borders. The rash can appear on any part of the body, but most commonly affects the knees, elbows, lower back and scalp. Rarer types of psoriasis may cause pus-filled blisters or a red, peeling rash. Plaques that have cleared often leave brown or pale marks that gradually fade.
Symptoms: Itching is mild in most patients, but can be severe. Scratching may cause skin thickening, and the patient may also experience painful skin cracks or fissures.
Treatment: Depending on the severity, symptoms may be managed using topical therapy, phototherapy, systemic therapy or targeted therapy. Symptoms can also be improved by avoiding smoking and reducing alcohol intake.
(Healthdirect 2023b; Jones et al. 2023)
Rosacea
Type: Chronic condition.
Cause: Unknown, but is thought to be related to genetic, environmental, vascular and inflammatory factors, along with a reaction to the demodex mite that lives on the skin. Symptoms may be exacerbated by factors such as stress, alcohol, heat, exercise and spicy foods.
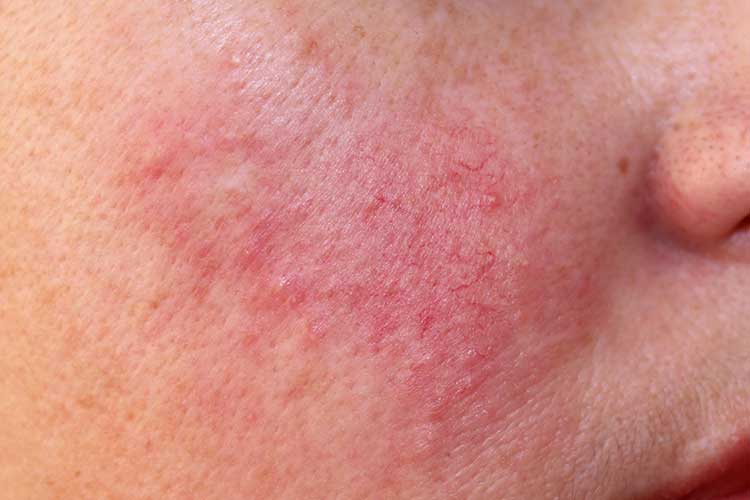
Rash appearance: Persistent redness and flushing that only affects the face, accompanied by enlarged capillaries. The rash may resemble a sunburn. In some cases, there might also be pimples on the forehead, cheeks and chin.
Symptoms:
Symptoms typically worsen with age and might include:
- Frequent blushing
- Bumps or pimples on the face that may cause a stinging or burning sensation
- Red or irritated eyes, or swollen eyelids
- Mild swelling on the cheeks or nose.
Treatment: Symptoms can be managed by avoiding known triggers, applying creams and gels, using diathermy to apply heat to damaged blood vessels and undergoing laser surgery to treat enlarged capillaries.
(Better Health Channel 2023b; Ciconte 2024)
Scabies
Type: Acute parasitic infection.
Cause: Infestation by Sarcoptes scabiei mites, which burrow under the skin and lay eggs. Scabies can be spread between people via direct contact.
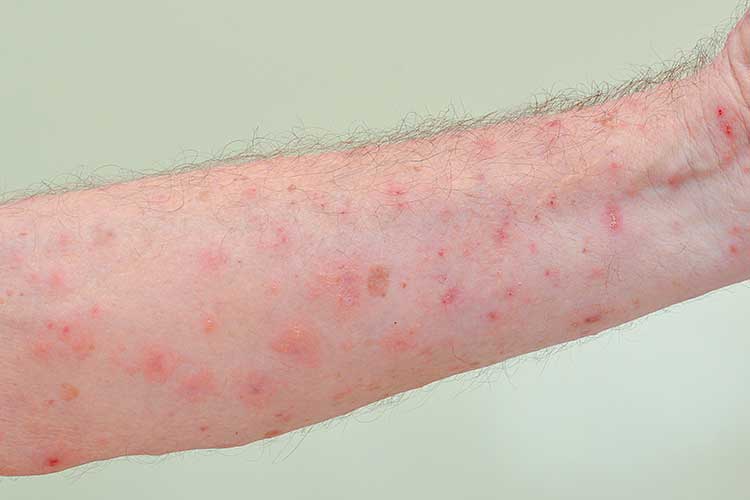
Rash appearance: Small red bumps that often form a line and may resemble hives, bites, knots or pimples. Sometimes the rash resembles scaly eczema patches. There may also be visible burrows in the affected areas. Commonly affected areas of the body include the wrists, fingers, armpits, elbows, buttocks and groin.
Symptoms: Intense itching that worsens at night and after hot baths and showers. Scratching may lead to infection.
Treatment: First-line treatment is generally the application of 5% permethrin cream or lotion, which is an insecticide used to kill parasites.
(Better Health Channel 2023c; AAD 2025; Stewart 2024)
Scarlet Fever
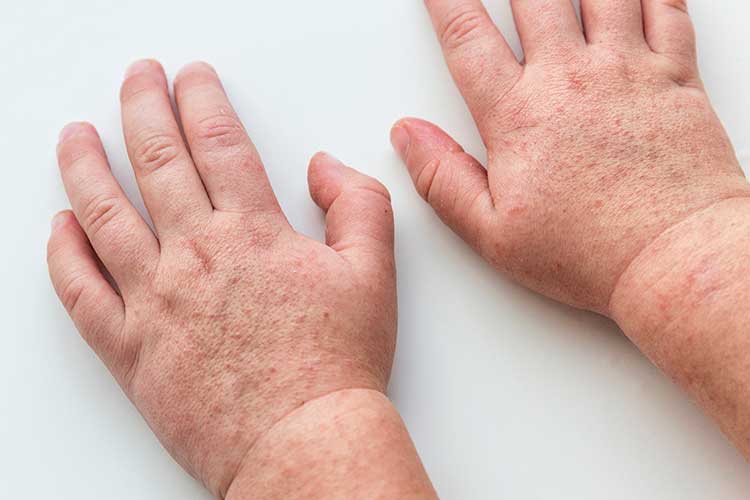
Type: Acute bacterial infection.
Cause: Infection by group A streptococci bacteria, the same bacteria that causes strep throat, impetigo and rheumatic fever. The bacteria is spread by coughing, sneezing or making contact with an infected person or contaminated surface. It predominantly affects children between the ages of 5 and 15.
Rash appearance: The rash initially presents as red blotches, most commonly on the face, neck, underarms or groin. Within 24 hours, the rash spreads to the rest of the body and changes to resemble a sunburn, with a sandpaper-like texture. Three to seven days later, the rash will peel.
Symptoms:
- Red sore throat and tonsils
- Swallowing difficulties
- Swollen glands
- Fever
- Red bumps on the tongue (‘strawberry tongue’)
- Headache
- Abdominal pain, nausea and vomiting
- Body aches.
Treatment: Antibiotics must be administered to prevent the bacteria from spreading and potentially causing serious complications like rheumatic fever, kidney disease, pneumonia or arthritis. Rest, pain relief and adequate hydration may assist in symptom management.
Further information: All About Strep Throat
(Healthdirect 2023c; Oakley 2015)
Varicella (Chickenpox)
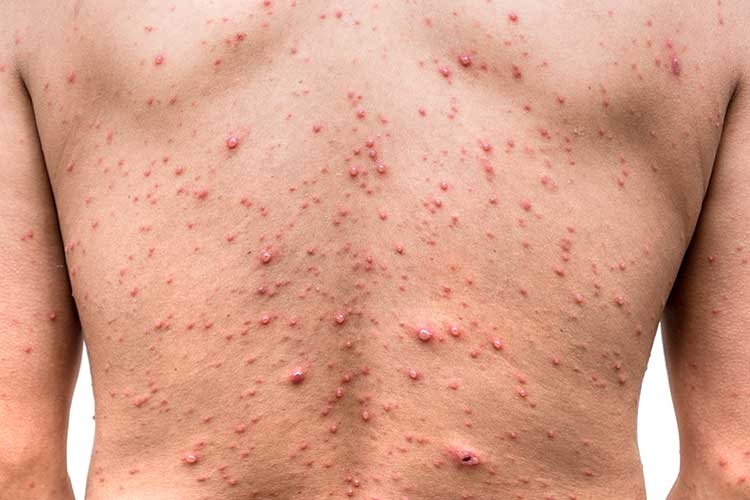
Type: Acute viral infection.
Cause: Infection with the varicella-zoster virus, which is spread by inhaling the particles dispersed when an infected person coughs or sneezes, or through touching the fluid from an infected person’s chickenpox blisters.
Rash appearance: Red rash that turns into fluid-filled blisters, which may then burst and crust over.
Symptoms:
- Itching
- Fever
- Headache
- Sore throat.
Treatment: Chickenpox is generally mild and will resolve on its own. Symptoms can be managed by resting, avoiding scratching, taking lukewarm baths with oatmeal, taking paracetamol and using creams or lotions to decrease itching.
(Healthdirect 2023d; Better Health Channel 2023d)
Skin Rash Red Flags
While some rashes are mild and don’t have any cause for concern, the following signs may indicate a serious illness and should be escalated immediately:
- Breathing difficulties, tight throat and swollen tongue, which indicate a severe allergic reaction
- Non-blanching rash, which might indicate severe illnesses such as sepsis or meningitis
- Fever
- Hypotension
- Severe pain
- The patient has recently started taking a new medicine
- The patient is immunosuppressed
- Rapid spreading of the rash
- Sudden onset of the rash
- Signs of infection
- The rash is affecting the entire body
- Abnormal bleeding or bruising under the rash
- Red streaks.
(Barrell & Bard 2021; HealthONE 2020; AAD 2024; Donaldson 2024; HealthEngine 2017)
Test Your Knowledge
Question 1 of 3
Which one of the following rashes is acute?
Topics
Further your knowledge
 Free
Free Free
Free Free
Free Free
Free Free
FreeReferences
- American Academy of Dermatology Association 2024, Rash 101 in Adults: When to Seek Medical Treatment, AAD, viewed 21 March 2025, https://www.aad.org/public/everyday-care/itchy-skin/rash/rash-101
- American Academy of Dermatology Association 2025, Scabies: Signs and Symptoms, AAD, viewed 21 March 2025, https://www.aad.org/public/diseases/a-z/scabies-symptoms
- Australasian Society of Clinical Immunology and Allergy 2024a, Anaphylaxis, ASCIA, viewed 21 March 2025, https://www.allergy.org.au/patients/about-allergy/anaphylaxis
- Australasian Society of Clinical Immunology and Allergy 2024b, Contact Dermatitis, ASCIA, viewed 21 March 2025, https://www.allergy.org.au/patients/skin-allergy/contact-dermatitis
- Australasian Society of Clinical Immunology and Allergy 2024c, Eczema (Atopic Dermatitis) Frequently Asked Questions (FAQ), ASCIA, viewed 21 March 2025, https://www.allergy.org.au/patients/skin-allergy/eczema
- Barrell, A & Bard, S 2021, ‘Causes for a Non-Blanching Rash in Adults and Children’, MedicalNewsToday, 27 January, viewed 21 March 2025, https://www.medicalnewstoday.com/articles/non-blanching-rash
- Better Health Channel 2022, Allergies to Bites and Stings, Victoria State Government, viewed 21 March 2025, https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/allergies-to-bites-and-stings
- Better Health Channel 2023a, Eczema (Atopic Dermatitis), Victoria State Government, viewed 21 March 2025, https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/eczema-atopic-dermatitis
- Better Health Channel 2023b, Rosacea, Victoria State Government, viewed 21 March 2025, https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/rosacea
- Better Health Channel 2023c, Scabies, Victoria State Government, viewed 21 March 2025, https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/scabies
- Better Health Channel 2023d, Chickenpox, Victoria State Government, viewed 21 March 2025, https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/chickenpox
- Ciconte, A 2024, Rosacea, Australasian College of Dermatologists, viewed 21 March 2025, https://www.dermcoll.edu.au/atoz/rosacea/
- Donaldson, R 2024, General Approach to Rashes, WikEM, viewed 21 March 2025, https://wikem.org/wiki/General_approach_to_rashes
- Healthdirect 2023a, Shingles, Australian Government, viewed 21 March 2025, https://www.healthdirect.gov.au/shingles
- Healthdirect 2023b, Psoriasis, Australian Government, viewed 21 March 2025, https://www.healthdirect.gov.au/psoriasis
- Healthdirect 2023c, Scarlet Fever, Australian Government, viewed 21 March 2025, https://www.healthdirect.gov.au/scarlet-fever
- Healthdirect 2023d, Chickenpox (Varicella), Australian Government, viewed 21 March 2025, https://www.healthdirect.gov.au/chickenpox
- Healthdirect 2024a, Insect Bites and Stings, Australian Government, viewed 21 March 2025, https://www.healthdirect.gov.au/insect-bites-and-stings
- HealthEngine 2017, When Should you See a Doctor About a Rash?, HealthEngine, viewed 21 March 2025, https://healthinfo.healthengine.com.au/when-should-you-see-a-doctor-about-a-rash
- HealthONE 2020, ‘When to Go to the ER For a Rash’, HealthONE Blog, 20 November, viewed 21 March 2025, https://healthonecares.com/blog/entry/when-to-go-to-the-er-for-a-rash
- Mayo Clinic 2022, Shingles, Mayo Clinic, viewed 21 March 2025, https://www.mayoclinic.org/diseases-conditions/shingles/symptoms-causes/syc-20353054
- National Cancer Institute 2020, Rash, U.S. Department of Health and Human Services, viewed 21 March 2025, https://www.cancer.gov/publications/dictionaries/cancer-terms/def/rash
- National Eczema Association 2025, What is Eczema?, NEA, viewed 21 March 2025, https://nationaleczema.org/eczema/
- Gartside, J 2024, Anaphylaxis, DermNet, viewed 21 March 2025, https://dermnetnz.org/topics/anaphylaxis
- Jones, C, Gupta, M, Uddin, S & Oakley, A 2023, Psoriasis, DermNet, viewed 21 March 2025, https://dermnetnz.org/topics/psoriasis
- Oakley, A 2015, Scarlet Fever, DermNet, viewed 21 March 2025, https://dermnetnz.org/topics/scarlet-fever
- Queensland Government 2019, Anaphylaxis, Queensland Government, viewed 21 March 2025, https://www.qld.gov.au/health/condition/accidents-injuries-and-poisonings/allergic-reactions/anaphylaxis
- The Royal Australian College of General Practitioners 2016, ‘Dermatological Presentations’, 2022 RACGP Curriculum and Syllabus for Australian General Practice, 6th edn, viewed 21 March 2025, https://www.racgp.org.au/education/education-providers/curriculum/curriculum-and-syllabus/units/dermatological-presentations
- The Royal Children's Hospital Melbourne 2018, Rashes, RCHM, viewed 21 March 2025, https://www.rch.org.au/kidsinfo/fact_sheets/Rashes/
- Skin Health Institute 2023, Occupational Contact Dermatitis, Skin Health Institute, viewed 21 March 2025, https://www.skinhealthinstitute.org.au/page/96/occupational-dermatitis
- Soyer, P & Lee, K 2018, ‘Common Skin Rashes and What to do About Them’, The Conversation, 21 March, viewed 21 March 2025, https://theconversation.com/common-skin-rashes-and-what-to-do-about-them-91518
- Stewart, M 2024, Permethrin Cream, Patient, viewed 21 March 2025, https://patient.info/medicine/permethrin-cream-lyclear
- Tate, B 2019, Irritant Contact Dermatitis (ICD), Australasian College of Dermatologists, viewed 21 March 2025, https://www.dermcoll.edu.au/atoz/irritant-contact-dermatitis-icd/
 New
New 
