Ask any nurse, and they will no doubt already know that when children and young people present to healthcare environments, they are faced with a range of emotions from fear to anxiety, all of which are potentially exacerbated by unfamiliar surroundings, people and equipment.
Compared to adults, children have fewer coping mechanisms. When experiencing pain or illness, their distress levels often escalate, causing a flow-on effect to not only parents and caregivers but healthcare providers alike (Stock et al. 2012). This is perhaps no more evident than when attempting painful or uncomfortable procedures, such as taking blood. In some circumstances, even obtaining vital signs may have negative emotional or behavioural consequences (Duff et al. 2011).
The chance of a nurse being involved in the care of a child that hasn’t resulted in tears at some stage is slim. However, by applying the use of age-appropriate language, as well as various distraction techniques, nurses and healthcare providers can successfully assist their paediatric patients through such procedures, resulting in the best patient outcomes.
Language
Explain the procedure. This reduces anxiety and any misconceptions by allowing the child to understand the purpose of the procedure rather than perceiving it as a form of punishment. Your explanation should be honest, developmentally appropriate, succinct and free of unnecessary details that can heighten anxiety (Stock et al. 2012). As children get older, involving them in the process and explaining intentions increases the child’s confidence, allows them to ask questions and makes them feel that their independence is being maintained throughout their care (Curtis & Ramsden 2012).
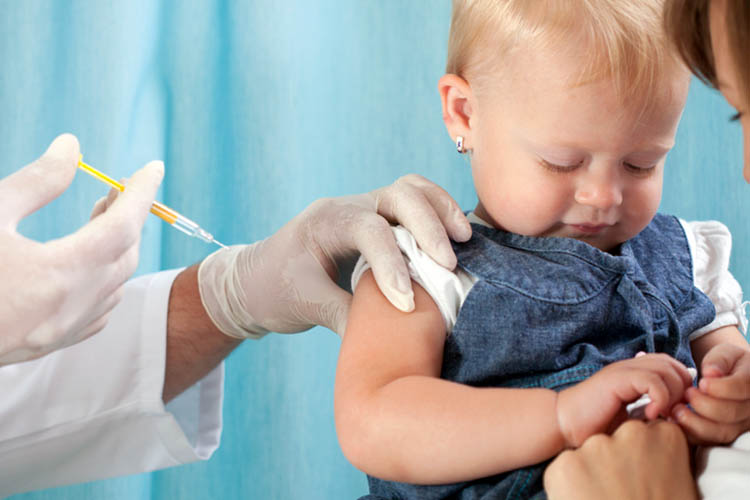
Avoid negative words. Words like ‘hurt’ and ‘sting’ when used during procedure preparation do not have any effect on reducing painful sensations and may induce greater distress before the procedure even takes place. It is recommended that these are instead replaced with affirmative language such as ‘this medicine will make you more comfortable’ or ‘the needle will help your body get better’ (Stock et al. 2012).
Give choices and empower. Children may feel like they have a loss of control in unfamiliar environments. This can further heighten anxiety, so offering choices such as, ‘Which arm would you like the blood pressure cuff on?’ can empower the child in a situation where many choices are already removed. Similarly, allowing children to play and become familiar with certain pieces of equipment - such as an oxygen mask - returns some feelings of control and reduces apprehension (Stock, Hill, and Babl 2012).
Distraction
Evidence strongly supports the use of distraction to reduce pain and distress during medical procedures in children. Duff et al. (2011) have identified two main principles:
- Attention can be shifted away from potentially distressing procedures via the use of age-appropriate activities.
- The more interactive and varied the chosen distraction technique is, the greater the cognitive need and, therefore, the greater the likelihood that distress levels are reduced.
Plummer (2016) recommends a variety of distraction approaches depending on the age and development stage of the child. These are all proven to be effective.
The Royal Children’s Hospital Non-Pharmacological Methods Of Pain Management
| Babies | Toddlers | Pre-School | School Age | Adolescents |
|---|---|---|---|---|
| Breastfeeding | Dummy, blanket, favourite toy | Blanket, favourite toy | Non-procedural talk about favourite topics | Non-procedural talk about favourite topics |
| Watching bubbles | Textured toys (e.g. squishy balls), imaginary play, popping bubbles | Textured toys (e.g. squishy balls), imaginary play, popping bubbles | Humour | Humour |
| Relaxed breathing of caregiver | 'Blowing the hurt away', blowing bubbles | 'Blowing the hurt away', blowing bubbles | Breathing and relaxation | Breathing and relaxation |
| Singing and music, music therapist | Singing and music, music therapist | Singing and music, music therapist | iPod, music therapist | iPod, music therapist |
| Sucrose and non-nutritive sucking | Computer game/DVD/iPad | Computer game/DVD/iPad | Computer game/DVD/iPad | Computer game/DVD/iPad |
| Rattle/shaker | Sound/pop-up books | ‘I Spy’/sound books | ‘I Spy’/’Where’s Wally’ | Prompt cards and conversation starters |
(Plummer 2016)
It is important to plan two to three options so that a new distractor can be introduced should the child become distressed, as well as to ensure the child does not remove focus from the distractor and attempt to look at the procedure. The positioning of the child and the procedure are important; a blanket or book may assist in shielding anxiety-provoking views in certain circumstances (Plummer 2016).
Conclusion
Ultimately, the building of trust between nurse and child and avoiding a negative hospital or healthcare experience is one of the main goals when nursing paediatric patients. Through effective communication techniques and applying some of the strategies discussed, this is not only achievable but will enable optimum assessment, management and interventions. Of course, there are many other strategies other than language and distraction that can be utilised, and with experience and exposure, each nurse can find their own individual way of communicating with children.
Topics
References
- Curtis, K & Ramsden, C 2011, Emergency and Trauma Care for Nurses and Paramedics, Elsevier Australia, Chatswood, NSW, Australia.
- Duff, A, Gaskell, S, Jacobs, K, & Houghton, J 2012, ‘Management of Distressing Procedures in Children and Young People: Time to Adhere to the Guidelines’, Archives of Disease in Childhood, vol. 97, no. 1, viewed 20 November 2023, https://www.researchgate.net/publication/51797413_Management_of_distressing_procedures_in_children_and_young_people_Time_to_adhere_to_the_guidelines
- Plummer, K 2016, 4.5.2 Psychological Interventions, The Royal Children’s Hospital Melbourne, viewed 20 November 2023, https://www.rch.org.au/uploadedFiles/Main/Content/rchcpg/hospital_clinical_guideline_index/PPM%204.5.2%20psychological.pdf
- The Royal Children’s Hospital Melbourne 2020, Procedure Management Guideline, RCHM, viewed 20 November 2023, https://www.rch.org.au/rchcpg/hospital_clinical_guideline_index/Procedural_Pain_Management/
- Stock, A, Hill, A, & Babl, F 2012, ‘Practical Communication Guide for Paediatric Procedures’, Emergency Medicine Australasia, vol. 24, no. 6, viewed 20 November 2023, https://onlinelibrary.wiley.com/doi/full/10.1111/j.1742-6723.2012.01611.x
 New
New 
